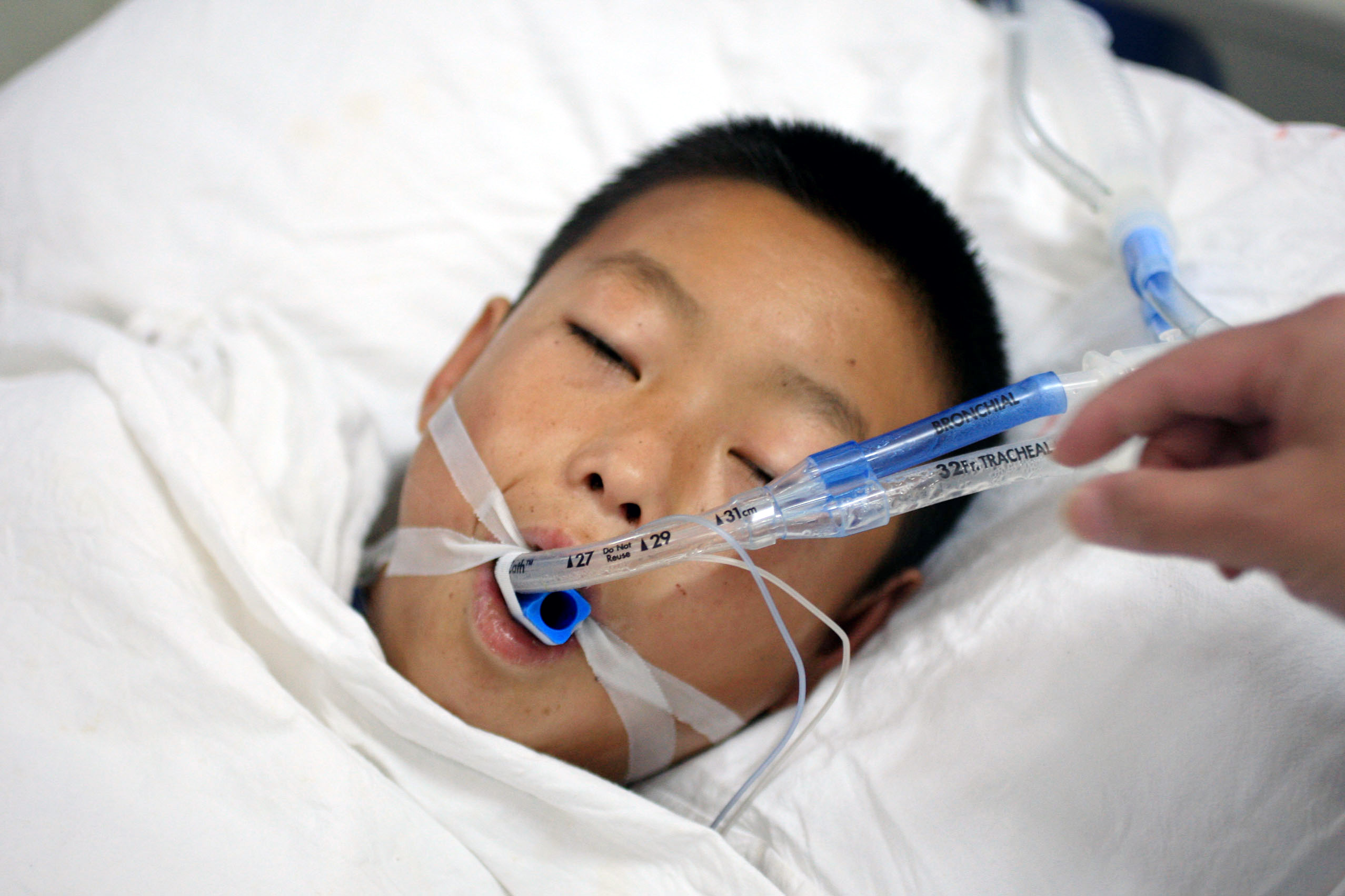
We provide exceptional pediatric and geriatric home health care services tailored to your unique needs. Whether your child or older patient with special need or complex care requires private-duty nursing, specialized therapy, or personal care assistance, our experienced team is here to support you every step of the way.
We believe in a patient-first approach, ensuring that your health and comfort are our top priorities. With dedication and commitment to excellence, we strive to deliver the highest quality care anytime, anywhere.